If you run an outpatient imaging center, you've probably already felt this one: EviCore just migrated prior authorization submissions for multiple Aetna Better Health state Medicaid plans — Texas, Virginia, Illinois, Michigan, and others — from the MedSolutions portal to the CareCore National portal.
Same credentials. Different portal. New CPT code lists effective January 1, 2026. And in some states like Ohio, EviCore stopped processing Aetna Better Health prior auth requests entirely.
Meanwhile, Cigna Medicare Advantage rebranded to HealthSpring under HCSC, and radiology, cardiology, and MSK requests now route through a different health plan name in the same EviCore system.
This isn't a one-time event. This is the new normal.
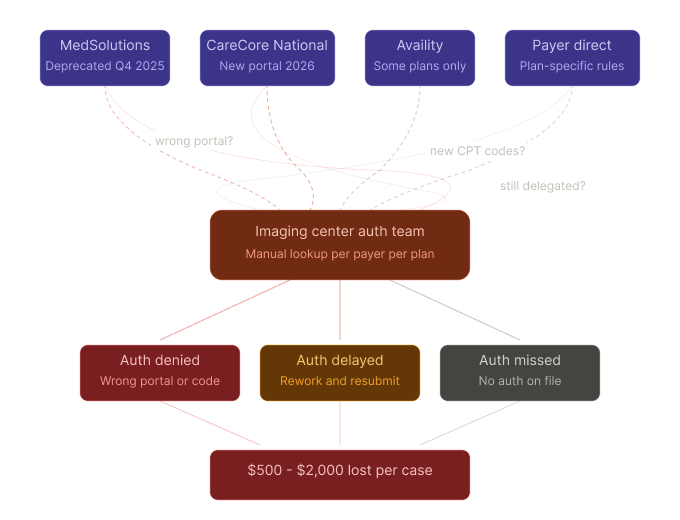
Every quarter, payers shift portals, update CPT code lists, change delegation partners, or restructure plan names. And every time they do, your front-desk staff and auth coordinators have to figure out: Where do I submit this now? Which codes changed? Is this plan even still delegated to EviCore?
Here's the problem — most imaging centers are still running this process manually. Staff members memorize which portal goes with which payer and plan. When something changes, they find out the hard way: a rejected submission, a delayed auth, a claim that gets denied because the authorization was never properly obtained.
The cost isn't just operational. It's financial.
A single missed or delayed prior auth on an MRI can mean $500–$2,000 in lost revenue per case. Multiply that across dozens of cases per week, and the leakage adds up fast.
This is exactly why we built Gravity Auth.
At Alpha Nodus, we work exclusively with outpatient diagnostic imaging centers and radiology practices. We see this pain every single day. Gravity Auth — part of our AI-first Gravity Platform — was designed to take the chaos out of prior authorization by solving the problems that portal shuffles like this one create:
Payer-aware routing. Gravity Auth knows which payer delegates to which utilization management vendor, which portal applies, and which CPT codes require authorization — so your team doesn't have to memorize it or find out the hard way when rules change.
Automated submission. Instead of your auth coordinators toggling between CareCore National, MedSolutions, Availity, and a dozen payer-specific portals, Gravity Auth handles the submission workflow from a single interface — pulling the right data from your RIS/EMR and routing it to the right destination.
Denial prevention at the point of entry. Gravity Auth flags missing documentation, incorrect codes, and routing mismatches before submission — not after a denial hits your accounts receivable 30 days later.
Real-time status tracking. No more calling payer phone lines or logging into five different portals to check auth status. Your team gets a unified view of every pending, approved, and denied authorization across all payers.
The payers aren't going to simplify this for you. EviCore alone manages prior auth across dozens of health plans, each with different portals, code lists, and delegation rules. That complexity is only increasing.
The imaging centers that thrive in this environment will be the ones that automate, accelerate, and amplify their prior authorization workflows — turning payer complexity into a solved problem instead of a daily fire drill.
That's what Gravity Auth does. And we're just getting started.